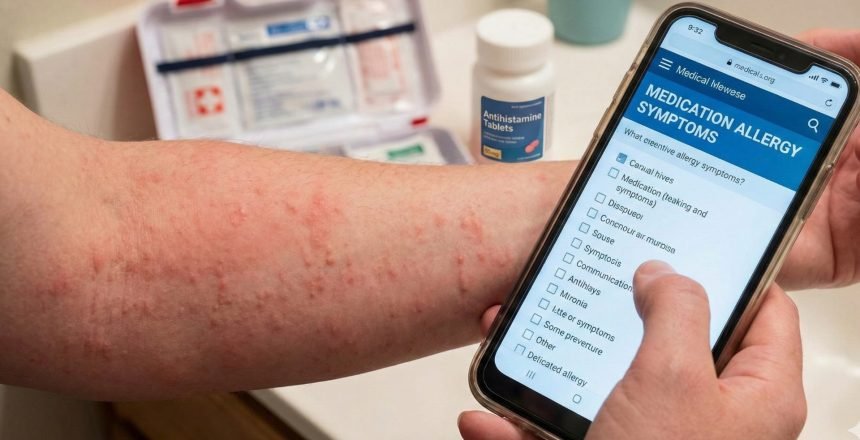
Allergic reactions to medications represent a significant health problem affecting millions of people each year. From mild skin rashes to potentially life-threatening emergencies, these reactions can vary enormously in severity and presentation. Recognizing the signs and symptoms of a drug allergy is fundamental for obtaining timely treatment and avoiding dangerous future exposures.
Understanding Drug Allergies: The Basics
A drug allergy is an adverse reaction of the immune system to a medication. It’s important to distinguish this from other side effects that don’t involve the immune system. When a person is truly allergic to a medication, their immune system mistakenly identifies the drug as a harmful substance and mounts a defensive response.
This distinction is crucial because approximately 10% of the population reports drug allergies, but studies have shown that many of these reported allergies aren’t true allergies but other types of adverse reactions. For example, stomach upset caused by an antibiotic is a predictable side effect, not an allergy. However, hives appearing after taking the same antibiotic does represent an allergic reaction.
The distinction matters for several reasons. True allergies can worsen with repeated exposure and may lead to severe reactions. They also typically require permanent avoidance of the drug and potentially related medications. Non-allergic side effects, while unpleasant, may be manageable or may not recur with subsequent exposures under different circumstances.
Drug allergies can develop at any time, even after having taken the same medication without problems previously. In fact, prior exposure is typically required for a true allergy to develop, as the immune system needs to be “sensitized” to the substance during the first exposure before it can mount an allergic response during subsequent exposures.
The sensitization process involves the immune system recognizing the drug (or a metabolite of the drug) as foreign, processing it, and creating antibodies or memory T-cells specific to that substance. This process can take days to weeks and doesn’t produce symptoms. It’s only upon re-exposure that the established immune response produces the clinical symptoms we recognize as an allergic reaction.
Medications Most Commonly Associated with Allergic Reactions
While any medication can potentially cause an allergic reaction, certain drugs are more frequent culprits.
Antibiotics, particularly penicillins and cephalosporins, top the list. Penicillin and its derivatives are the most common cause of reported drug allergies. However, it’s important to note that many people who believe they’re allergic to penicillin actually aren’t; studies show that up to 90% of people with reported penicillin allergies can tolerate it when properly tested.
This discrepancy occurs for several reasons. Childhood reactions may have been non-allergic (such as viral rashes coinciding with antibiotic use), immune systems can change over time resulting in loss of sensitization, or family lore about “allergies” may be inaccurate. Additionally, many reported “penicillin allergies” stem from side effects like gastrointestinal upset rather than true immune-mediated reactions.
Non-steroidal anti-inflammatory drugs (NSAIDs) like aspirin, ibuprofen, and naproxen also frequently cause allergic and pseudo-allergic reactions. These can range from respiratory reactions (asthma, nasal polyps) to urticaria and angioedema, to severe cutaneous reactions.
Anticonvulsants (particularly aromatic anticonvulsants like phenytoin, carbamazepine, and phenobarbital), certain chem
otherapy agents, biologic medications used for autoimmune diseases, and some anesthetics are also associated with higher rates of allergic reactions.
Sulfonamide antibiotics (often called “sulfa drugs”) are another common cause of drug allergies. These should be distinguished from non-antibiotic sulfonamides like furosemide or sulfonylurea diabetes medications, which have a different chemical structure and generally don’t cross-react.
Allopurinol, used for gout, can cause severe cutaneous reactions, particularly in certain populations with specific genetic risk factors. Antiretroviral medications for HIV, particularly abacavir and nevirapine, are associated with hypersensitivity reactions that can be severe.
Topical medications applied to the skin, such as neomycin or benzocaine, can cause allergic contact dermatitis, a different form of immune reaction that typically develops more slowly than immediate hypersensitivity reactions.
Contrast dyes used in imaging procedures can cause reactions that resemble allergies, though most are actually non-immune-mediated reactions. However, they can still be serious and require similar management approaches.
Types of Allergic Reactions: From Type I to Type IV
Immunologists classify allergic reactions to medications into four types based on the underlying immune mechanism. This classification helps understand why reactions can look and feel different.
Type I reactions are mediated by IgE antibodies and occur rapidly, typically within minutes to hours after exposure to the medication. These are the “classic” allergic reactions most people imagine and include symptoms like hives, swelling, wheezing, and, in severe cases, anaphylaxis.
The mechanism involves mast cells and basophils that have IgE antibodies bound to their surface. When the drug binds to these antibodies, it cross-links them, triggering massive release of histamine and other mediators. This causes vasodilation, increased vascular permeability, smooth muscle contraction, and mucus secretion – the physiological changes that produce the clinical symptoms we observe.
Type II reactions involve IgG or IgM antibodies that attack cells in the body that have been modified by the medication, potentially causing destruction of red blood cells, platelets, or white blood cells. These reactions may not be immediately obvious and can manifest as anemia, abnormal bleeding, or recurrent infections.
Drug-induced immune thrombocytopenia, drug-induced hemolytic anemia, and drug-induced agranulocytosis are examples of Type II reactions. They typically develop after several days to weeks of drug exposure and may persist for some time after the drug is discontinued, as the antibodies remain in circulation.
Type III reactions occur when immune complexes form between the drug and antibodies, depositing in tissues and causing inflammation. Serum sickness is a classic example, characterized by fever, rash, joint pain, and lymph node swelling, typically developing 7-21 days after exposure.
Historically, serum sickness occurred after administration of animal-derived antisera (hence the name). Today, drug-induced serum sickness or serum sickness-like reactions can occur with various medications, including antibiotics, particularly beta-lactams and sulfonamides.
Type IV reactions are mediated by T-cells and develop more slowly, typically 48-72 hours after exposure. Allergic contact dermatitis is the most common example, but more severe reactions like Stevens-Johnson syndrome also fall into this category.
In Type IV reactions, T-cells recognize the drug (or drug-hapten complex) presented by antigen-presenting cells. These sensitized T-cells then proliferate and release inflammatory cytokines, causing tissue damage. The delayed time course reflects the time needed for T-cell activation and accumulation at the reaction site.
Signs and Symptoms: What to Look For
Symptoms of an allergic reaction to medications can affect multiple body systems and vary widely in severity.
Cutaneous manifestations are the most common. Urticaria or hives appear as raised, red, swollen, itchy welts on the skin that can vary in size and location. They typically appear and disappear within hours, moving to different body areas. These lesions are intensely itchy and have well-defined borders.
Individual urticarial lesions typically last less than 24 hours in any one location, though new lesions may continually appear. This transient nature helps distinguish urticaria from other rashes that remain fixed in location. Pressing on the center of an urticarial lesion typically causes blanching (temporary whitening), another distinguishing feature.
Maculopapular rashes consist of flat red areas with small raised bumps. Unlike hives, these rashes tend to be more symmetrical and persistent, often starting on the trunk and spreading toward the extremities. They may cause variable itching and typically appear 3-10 days after starting the medication.
This type of rash often begins as small discrete lesions that can coalesce into larger patches. The face, trunk, and proximal extremities are commonly affected first. The rash may be associated with mild fever and malaise but generally isn’t accompanied by systemic toxicity unless it represents a more serious condition.
Angioedema involves swelling in deeper layers of the skin and generally affects the lips, tongue, eyelids, and hands or feet. Unlike superficial hives, angioedema can be painful rather than itchy and can affect the airways or gastrointestinal tract, causing difficulty breathing or abdominal pain.
Angioedema develops over minutes to hours and resolves more slowly than urticaria, often persisting for 24-72 hours. The swelling is typically non-pitting and may be asymmetric. When it involves the tongue, throat, or larynx, it can be life-threatening due to airway obstruction.
Respiratory symptoms include wheezing, difficulty breathing, chest tightness, persistent cough, and a sensation of throat constriction. These symptoms can progress rapidly and require urgent medical attention.
Bronchospasm (constriction of the airways) produces wheezing and shortness of breath. Laryngeal edema (swelling of the voice box) can cause voice changes, stridor (high-pitched breathing sound), and progressive airway obstruction. These respiratory manifestations can be life-threatening and constitute medical emergencies.
Gastrointestinal symptoms may include nausea, vomiting, diarrhea, and abdominal cramping. Although these symptoms are common as non-allergic side effects of many medications, when they occur alongside cutaneous or respiratory symptoms, they may indicate an allergic reaction.
In an allergic context, gastrointestinal symptoms result from mast cell activation in the GI tract, causing increased intestinal secretions, smooth muscle contraction, and increased motility. The symptoms typically develop rapidly, within minutes to hours of drug exposure.
Systemic symptoms such as fever, general malaise, lymph node swelling, and joint pain can accompany more severe allergic reactions or form part of syndromes like serum sickness or DRESS syndrome.
Cardiovascular symptoms may include a sudden drop in blood pressure, dizziness or lightheadedness, rapid or weak pulse, and feeling faint. These symptoms suggest anaphylaxis and require immediate emergency intervention.
Anaphylaxis: The Medical Emergency
Anaphylaxis represents the most severe form of allergic reaction and constitutes a medical emergency requiring immediate treatment. This potentially life-threatening systemic reaction can develop within minutes to hours after medication exposure.
Signs of anaphylaxis include severe breathing difficulty or audible wheezing, swelling of the tongue or throat making it difficult to swallow or breathe, sudden drop in blood pressure manifested as extreme dizziness, weakness, or fainting, rapid or weak pulse, confusion or altered consciousness, severe nausea, vomiting, or diarrhea, and widespread hives or skin flushing.
Anaphylaxis is defined by the rapid onset of symptoms involving multiple organ systems. Diagnostic criteria include acute onset of an illness with involvement of skin/mucosal tissue plus either respiratory compromise or reduced blood pressure, or two or more of the following: skin/mucosal involvement, respiratory compromise, reduced blood pressure, or persistent gastrointestinal symptoms.
The pathophysiology involves massive, widespread mast cell and basophil degranulation, releasing enormous quantities of histamine, tryptase, and other mediators into the circulation. This causes systemic vasodilation and increased vascular permeability (leading to shock), bronchospasm (causing respiratory distress), and activation of other inflammatory cascades.
Anaphylaxis requires immediate administration of epinephrine, usually via an autoinjector like EpiPen. Time is critical in these situations; delays in treatment can result in serious or fatal consequences. Even if symptoms improve after epinephrine, immediate transport to a hospital is necessary because a biphasic reaction can occur where symptoms return hours later.
The standard epinephrine dose for anaphylaxis is 0.3-0.5 mg intramuscularly in the anterolateral thigh. The injection can be given through clothing if necessary. The mid-outer thigh is preferred because it provides rapid, reliable absorption. Epinephrine begins working within minutes, constricting blood vessels, relaxing airway smooth muscle, and reducing mediator release.
Approximately 20% of anaphylactic reactions are biphasic, with symptoms recurring 1-72 hours after the initial reaction resolves. This is why observation in a medical facility for at least 4-6 hours after treatment is essential. Risk factors for biphasic reactions include severe initial presentations, delayed epinephrine administration, and inadequate initial treatment.
After the acute crisis, patients require evaluation by an allergist, prescription of an epinephrine autoinjector if they don’t already have one, education about recognition and self-treatment of anaphylaxis, and guidance about avoiding the culprit medication and potentially cross-reactive drugs.
Delayed Reactions and Serious Conditions
Some allergic reactions to medications develop days or even weeks after starting the medication and can be particularly severe.
Stevens-Johnson syndrome (SJS) and its more severe form, toxic epidermal necrolysis (TEN), are rare but potentially life-threatening cutaneous reactions. These conditions are characterized by widespread separation of the top layer of skin, creating lesions similar to severe burns.
Warning signs include high fever appearing before or alongside the rash, painful rash starting on the trunk and face before spreading, blisters on skin and mucous membranes including mouth, eyes, and genitals, skin peeling leaving raw, red areas, severe eye pain or light sensitivity, and a general feeling of severe illness.
SJS/TEN typically begins with a prodrome of fever, sore throat, and flu-like symptoms for 1-3 days. This is followed by development of painful, dusky-red or purpuric macules that rapidly progress to blistering and epidermal detachment. Nikolsky’s sign (lateral pressure causing skin to separate from underlying layers) is positive.
The distinction between SJS and TEN is based on the percentage of body surface area with epidermal detachment: SJS affects less than 10%, SJS-TEN overlap affects 10-30%, and TEN affects more than 30%. Mortality increases with extent of involvement, with TEN carrying a mortality rate of 25-30% despite optimal treatment.
These conditions require immediate hospitalization, typically in a burn unit or intensive care unit. Treatment involves discontinuation of all potentially causative medications, supportive care including fluid and electrolyte management, wound care, pain control, nutritional support, and prevention of secondary infections. Immunomodulatory therapies such as intravenous immunoglobulin (IVIG), corticosteroids, or cyclosporine may be used, though evidence for their efficacy is debated.
Complications can include secondary infections, sepsis, acute respiratory distress syndrome, gastrointestinal bleeding, and long-term sequelae such as scarring, pigmentation changes, and ocular complications including blindness. Survivors often require long-term ophthalmologic follow-up due to risk of chronic eye problems.
DRESS syndrome (Drug Reaction with Eosinophilia and Systemic Symptoms) is another severe reaction that typically develops 2-8 weeks after starting certain medications. DRESS combines cutaneous manifestations with internal organ involvement.
Symptoms include persistent high fever, extensive rash that may become pustular or exfoliative, prominent facial swelling, lymph node swelling in multiple areas, and involvement of internal organs, especially the liver. Laboratory findings typically include eosinophilia (elevated eosinophils), atypical lymphocytosis, and elevated liver enzymes.
The pathophysiology of DRESS involves T-cell-mediated reaction, often with reactivation of human herpesvirus 6 (HHV-6) and sometimes other herpesviruses. This viral reactivation may contribute to the severity and prolonged course of the syndrome.
DRESS has a mortality rate of approximately 10%, usually due to liver failure or other organ involvement. Treatment involves immediate discontinuation of the offending drug and supportive care. Systemic corticosteroids are often used, though optimal dosing and duration are uncertain. The syndrome can have a prolonged course, with symptoms sometimes persisting or recurring for weeks to months even after the drug is stopped.
Medications most commonly associated with DRESS include aromatic anticonvulsants (phenytoin, carbamazepine, phenobarbital), allopurinol, sulfonamides, dapsone, and minocycline. Some antiretroviral medications and antibiotics can also cause DRESS.
Acute generalized exanthematous pustulosis (AGEP) is another severe cutaneous reaction characterized by the rapid appearance of numerous small, sterile pustules on an erythematous base, typically starting in intertriginous areas and spreading. Fever is common. Unlike DRESS, AGEP usually resolves quickly (within 2 weeks) after drug withdrawal.
What to Do If You Suspect an Allergic Reaction
If you experience symptoms suggesting an allergic reaction to a medication, immediate steps are crucial.
For mild symptoms like isolated hives without other symptoms, stop the medication and contact your doctor or pharmacist immediately. Don’t take another dose before receiving medical guidance. Document the specific medication, dose, when you took it, and what symptoms you experienced.
Taking photographs of rashes can be helpful, as some reactions are transient and may not be visible during the medical evaluation. Note the timing of symptom onset relative to medication administration, any factors that seemed to worsen or improve symptoms, and any treatments you used.
For moderate symptoms including extensive hives, mild facial swelling, or significant gastrointestinal symptoms, seek medical attention the same day. You may need treatment with antihistamines or corticosteroids.
Healthcare providers may prescribe oral antihistamines (like diphenhydramine or cetirizine) to relieve itching and reduce hives. Corticosteroids (like prednisone) may be prescribed for more severe reactions to reduce inflammation and prevent progression. These medications treat symptoms but don’t address the underlying allergy.
For severe symptoms including any breathing difficulty, significant swelling of tongue or throat, severe dizziness, or any signs of anaphylaxis, call emergency services immediately. If you have an epinephrine autoinjector available, use it without delay.
Don’t wait to see if symptoms improve on their own. Anaphylaxis can progress rapidly, and early epinephrine administration improves outcomes. After using epinephrine, still seek emergency care, as observation and potential additional treatment are necessary.
After any allergic reaction to a medication, it’s important to obtain clear documentation of the incident. Ask your doctor about allergy testing if appropriate, ensure the allergy is clearly documented in your medical record, obtain a list of safe alternative medications you can use in the future, and consider wearing a medical alert bracelet or necklace if you’ve had severe reactions.
Allergy testing for drug allergies is available for some medications, particularly penicillin. Skin testing can help determine if you’re truly allergic or if the allergy label can be safely removed. For penicillin specifically, comprehensive evaluation including skin testing and sometimes graded challenge can determine whether you can safely use penicillin and related antibiotics in the future.
This is particularly important because unnecessarily avoiding penicillin can lead to use of broader-spectrum, more expensive, and potentially more toxic alternative antibiotics. Studies show that most people labeled as penicillin-allergic can safely tolerate penicillin when properly evaluated.
Preventing Future Reactions
Once you’ve experienced an allergic reaction to a medication, preventing future exposures is crucial.
Always inform all healthcare professionals, including doctors, dentists, pharmacists, and emergency personnel, about any known drug allergies. Provide specific details about which medication caused the reaction and what symptoms you experienced.
Simply stating “drug allergy” isn’t sufficient. Healthcare providers need to know the specific drug name, the type of reaction, the severity, and how long ago it occurred. This information helps them assess risk and choose appropriate alternatives.
Maintain an updated list of all your drug allergies and carry it with you or store it on your phone. Be specific: don’t just note “antibiotic allergy” but the exact name of the antibiotic.
Digital health records and smartphone apps can help maintain this information. Some apps allow you to store allergy information, medication lists, and emergency contacts in one place, accessible even when you’re unable to communicate.
Be cautious with related medications. If you’re allergic to penicillin, certain other beta-lactam antibiotics like some cephalosporins may pose a risk of cross-reaction. Your doctor can help you understand which medications to avoid.
Cross-reactivity patterns are complex. For penicillin-allergic patients, the risk of reacting to first-generation cephalosporins is approximately 10%, but the risk with later-generation cephalosporins is much lower (1-2%). Carbapenems and monobactams have different cross-reactivity patterns. An allergist can provide guidance tailored to your specific situation.
For severe allergies, consider carrying an epinephrine autoinjector and ensure that family members, close friends, and coworkers know how to use it. Check expiration dates regularly and replace as needed.
Two injectors are often prescribed because some reactions require a second dose. Store epinephrine at room temperature away from light, and check it periodically – if the solution appears discolored or contains particles, it should be replaced.
Before any medical procedure, surgery, or dental work, remind providers about drug allergies. These situations often involve multiple medications, and clear communication prevents accidental exposure to allergens.
In emergency situations, medical alert jewelry can communicate critical allergy information to first responders when you may be unable to do so yourself. Bracelets or necklaces engraved with “Drug Allergy” and the specific drug(s) can be life-saving.
Distinguishing True Allergies from Other Reactions
Not every adverse reaction to a medication is an allergy. This distinction matters because unnecessarily avoiding medications can limit your treatment options and potentially lead to less effective or more expensive therapies.
Predictable side effects like nausea from antibiotics or drowsiness from antihistamines aren’t allergies. Intolerances, such as stomach upset that consistently occurs with a medication but without immune involvement, also aren’t true allergies.
Drug intolerance refers to adverse effects at therapeutic doses in the absence of immune involvement. These effects may be related to the drug’s pharmacological actions or individual patient factors like age, genetics, or comorbidities.
Toxicity occurs when drug levels are too high, either due to excessive dosing or impaired elimination. Symptoms are typically dose-dependent and resolve when the drug level decreases.
Idiosyncratic reactions are unpredictable adverse effects that occur in a small subset of individuals, often related to genetic variations in drug metabolism. These aren’t immune-mediated but may be confused with allergies.
If you’re uncertain whether a past reaction was a true allergy, consider discussing with your doctor the possibility of evaluation by an allergist. Drug allergy testing can determine if you’re truly allergic, potentially “de-labeling” false allergies and expanding your treatment options safely.
Penicillin allergy evaluation is particularly important and well-established. A comprehensive evaluation typically includes detailed history, skin testing with both major and minor determinants, and sometimes an oral challenge with amoxicillin. This process can safely determine whether penicillin can be used in over 95% of patients labeled as allergic.
For other drugs, testing options are more limited. Direct skin testing is unreliable for most non-beta-lactam drugs. Drug provocation testing (giving the drug under controlled medical observation) may be performed in select cases when the benefits of determining tolerance outweigh the risks.
Special Populations
Certain populations require special considerations regarding drug allergies.
Children may outgrow some drug allergies, particularly those that occurred in early childhood. Many childhood “drug allergies” are actually viral rashes that coincided with antibiotic use. Pediatric allergists can help clarify whether reactions were truly allergic and whether children have outgrown sensitivities.
Elderly patients may have accumulated multiple drug allergy labels over their lifetimes. Given age-related changes in pharmacokinetics and the likelihood of polypharmacy, careful review of allergy histories is particularly important in this population to ensure they have access to optimal medications.
Pregnant women need special consideration, as both the avoidance of potentially necessary medications and the use of less-studied alternatives carry risks. Allergists and maternal-fetal medicine specialists can help balance these considerations.
Patients with atopic conditions (asthma, eczema, allergic rhinitis) may have a higher propensity for drug allergies, though having atopic disease doesn’t mean every adverse drug reaction is allergic.
Patients with HIV/AIDS have significantly higher rates of drug hypersensitivity reactions, particularly to sulfonamides. Desensitization protocols may be necessary for essential medications.
Conclusion
Recognizing the signs of an allergic reaction to medication empowers patients to seek appropriate care quickly and prevent dangerous future exposures. Although drug allergies can be concerning, with proper knowledge, clear documentation, and open communication with healthcare providers, they can be managed effectively while maintaining access to safe and effective medical treatments.
The key points to remember: allergic reactions can range from mild to life-threatening, immediate recognition and appropriate response are crucial for severe reactions, accurate documentation of drug allergies helps prevent future exposures while avoiding unnecessary medication restrictions, many reported drug allergies aren’t true allergies and can be safely evaluated and potentially de-labeled, and working with healthcare providers and allergists ensures you have access to the safest and most effective medications for your needs.
Understanding the signs and symptoms, knowing when to seek immediate help, and maintaining clear communication about drug allergies are essential skills for navigating modern healthcare safely. While the complexity of drug allergies can seem overwhelming, the combination of patient awareness, medical expertise, and advancing diagnostic capabilities makes it possible to manage these challenges effectively and ensure optimal therapeutic outcomes.